How do you investigate the mechanisms of COVID-19 disease?
There is an increasing emergence of previously unknown pathogens and antimicrobial resistance. COVID-19 has been an exemplar of the requirement for more rapid understanding and therapeutic design against novel pathogens.
The lung is the only internal organ directly subject to the environment and is therefore particularly vulnerable to pathogens. This, together with the increasing emergence of novel pathogens and antimicrobial resistance, has resulted in lower respiratory infections being a leading cause of death worldwide.
However, the likelihood of new pulmonary therapeutics reaching the market is only 3% compared to 6-14% for other disease therapeutics. This extremely high attrition rate can be partly attributed to the lack of reliable, predictive preclinical models that capture the intricacies of the human lung.
Our solution
Our two perfused multi-cell Lung-on-a-chip (alveolar and bronchial airway) models map the distinct physiology of the human lung, making it possible to study the mechanism of SARS-CoV-2 infection for drug screening, drug response, host-pathogen interactions, and immune response.
Our models show improved differentiation of alveolar and bronchial cells into physiologically relevant phenotypes that provide superior tissue formation and differentiation into key cell types found in the human lung.
PhysioMimix® COVID-19 Assays offer the possibility to study infection of the upper and lower airway. The co-cultures of epithelial and endothelial cells with multiple immune cell populations, including recirculating immune cells, accurately recapitulate the viral life cycle and host response.

This application was developed using funding from InnovateUK
Studying COVID-19
Limitations with current techniques
- The lung biology and immunology of animal models vary from humans
- Inability to track specific immune responses to pathogens
- Simple cell models (e.g. VeroE6) only model virus entry and replication
- Animals are needed to look at the systemic effects of infection
Advancements with PhysioMimix OOC
- Our lung models infected by SARS-CoV-2 produce physiologically-relevant inflammatory responses for therapeutic testing
- Complex co-culture provides phenotypes that reflect human physiology and immunology
- Ability to add multiple human immune cells (tissue-specific and circulating)
- Understand the basic virology, biology, and immunology of SARS-CoV-2 infection in humans
- Lung models can be connected to other organ systems to study multi-organ effects
End point measurements
Longitudinal and endpoint measurements include but not limited to:
Functionality biomarkers
- Production of mucus (bronchial model)
- Alcian blue – histology or colorimetric assay
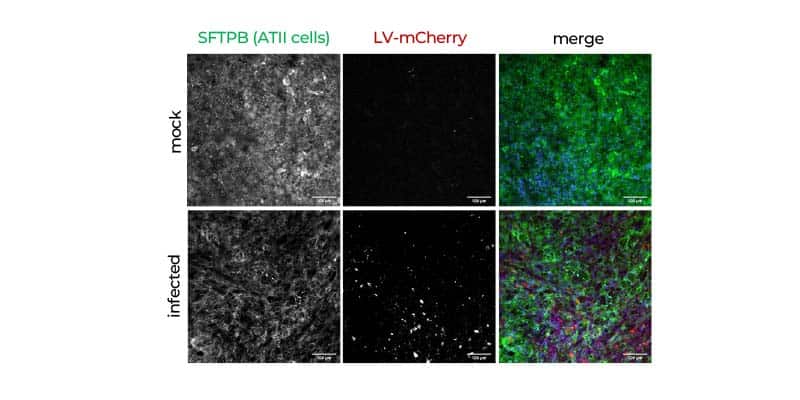
- Production of surfactant (alveolar model)
- qPCR
Profiling analysis
- Barrier integrity (TEER)
- Epithelial cellular composition
- Microscopy or qPCR
- Lactose dehydrogenase (LDH) release
- Adenosine Triphosphate (ATP)
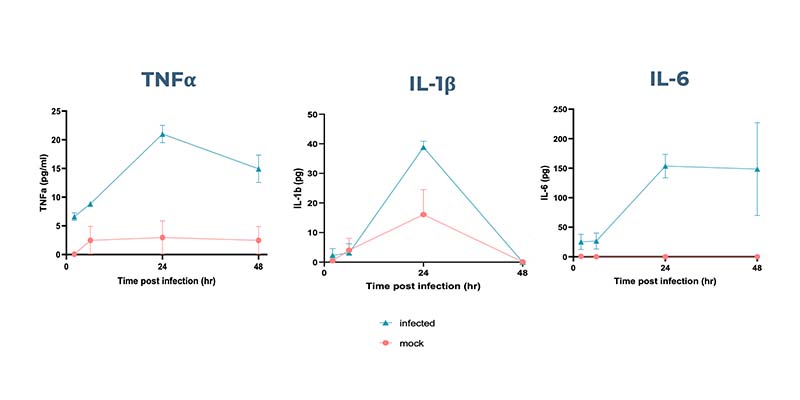
- Inflammatory response profiling
- Cytokine & chemokine immunoassays
- Confocal microscopy
- Transcriptomics
- Cellular phenotypes
- Viral receptor expression
- Genetic perturbations
Infection biomarkers
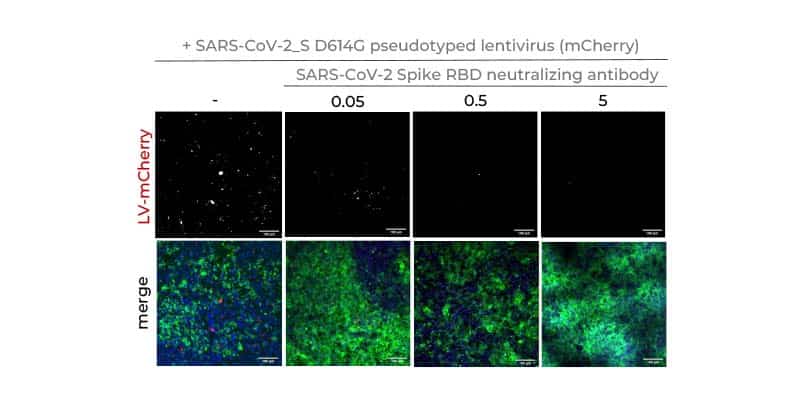
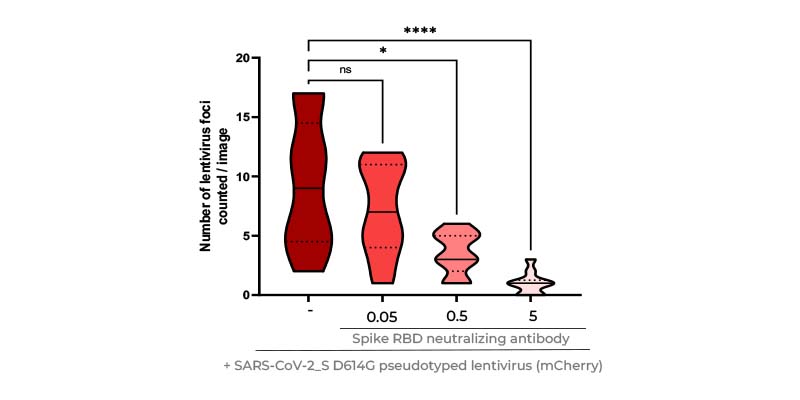
- Quantification of viral antigen
- Confocal microscopy immunofluorescence staining
- qPCR
- Transcriptomics
Explore our Lung-on-a-chip models
Recreate the airway or alveolar niche by culturing epithelial and endothelial cells on each side of an insert at ALI. Achieve a human-relevant barrier with enhanced functionality for longer term culture.
Add PhysioMimix OOC into your lab
Harness the power of PhysioMimix OOC in your own lab with the purchase of a single- or multi-organ microphysiological system.
With a growing community of users and support from our experts, there has never been a better time to transition into 3D cell culture.